Does Rheumatoid Arthritis Cause Hives?
The effect of rheumatoid arthritis (RA) is systemic, though it primarily affects the joints. Systemic means it can affect many parts of the body, not only the joints. For example, it can also cause skin problems. Can it also cause hives, a raised-itchy nettle rash on the skin?
Also called as ‘urticaria’, it is a skin reaction that leads to itchy nettle rash. It can range in size from tinny spots (a few millimeters in diameter) to large blotches as large as your hand (several inches in diameter). It may appear suddenly on a small area of the skin or affect across large areas, depending on the severity of the problem.
Symptoms and risk factors
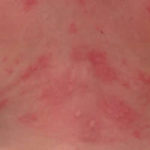 The symptoms of itchy nettle rash associated with hives include:
The symptoms of itchy nettle rash associated with hives include:
- It often results in pinkness or redness. Sometimes it may also be flesh-colored.
- It can be intensely itchy.
- The shape of the spot is usually like a worm or roughly oval.
- And again, the size can vary from several inches across or less than one inch in diameter.
The risk factors, conditions /factors that increase your risk of developing hives, are as follows:
- If you have a personal history of hives before.
- A family history of the same condition might also have an effect, especially for first relatives such as father, mother, brother, or sister.
- If you are an allergy sufferer. The problem is often triggered by allergic reactions.
- Particular health conditions such as thyroid disease, lupus, or lymphoma.
Hives is common, and having some of risk factors mentioned above can put you at higher risk than others.
It can be acute (mostly) or chronic. Acute or short-term hives can affect about 1 out of 5 people at some point in their lives. Chronic or long-term hives is less common, but it is more difficult to treat.
Causes
Some people have hives when a trigger leads to high levels (higher than normal) of histamine and other certain chemicals in the skin.
Histamine is a chemical released by the body immune system. Its function is similar to a bouncer at a club. It can help your body to drive away something that bothers you a lot, including those that seem harmless in some cases.
Histamine can stimulate your heart to boost more blood flow to the affected area. This results in inflammation, allowing other chemicals of your immune system to perform ‘repair work’.
But in some people, the release of histamine is overactive. And this overreaction can be counterproductive.
If you have allergy, a chain reaction of your immune system starts running when you come across your allergen. First, a signal is delivered to your mast cells. The message is an ‘order’ to release more histamine stored in those cells.
Then there will be more blood flow to the area affected by allergen, and inflammation forms. Histamine and other chemicals also cause the blood vessels to open up. The result, you may have hives.
High levels of histamine in the skin, which eventually may trigger acute hives, occur for many reasons. Allergic reaction to allergen is one of the main ones, these include:
- Allergic reaction to particular foods – cheese, eggs, peanut, wheat, milk (dairy products), and shellfish are for examples.
- Allergy related to particular environmental factors, including; chemicals, pet dander, dust mites, and pollen.
- Sometimes some people have hives when they get exposure to latex. This is common in healthcare workers.
Other possible answers are:
- Bad water, heat, sunlight, or cold exposure.
- Emotional stress or physical triggers (such as exercise and pressure on the skin).
- Infections, from mild infection (like cold) to more serious infection (like HIV).
- Insect stings or bites.
- Side effect of certain medications. The common culprits are some blood pressure medications, naproxen, ibuprofen, aspirin, NSAIDs, antibiotics, and penicillin. The effect of those medicines can vary from person to person. In other words, not all people who take them definitely develop hives.
In some cases, the cause of acute hives is unidentifiable. The good news, it is usually mild (not serious) – and relatively easier to treat. The appearance of the affected skin may change within 24 hours, and it often settles within a few days or weeks.
RA is one of common types of arthritis, though it is less common than osteoarthritis. It occurs when the body immune system attacks the lining of the protective membranes surrounding the joints called ‘synovium’.
So in RA, there is something that goes awry with the body immune system. Therefore it’s also known as autoimmune disease.
Still, it mainly affects and attacks your joints. But again the effect of the disease is systemic. In other words, it can affect other parts /organs of your body that have nothing to do with your joints, including skin.
For more information about the link between RA and skin problems, you might also like to read:
- How does RA affect your skin?
- Can it also cause itchy skin?
- Can it make you sweat?
- About rheumatoid nodules
Chronic hives is not as common as acute hives. It is a condition of when the itchy nettle rash becomes chronic (come & go) or persists for more than 6 weeks. Even sometimes, it may persist over many years.
It is quite rare, but it could be more painful and serious, because it is often linked to particular health condition. The main culprit is the abnormality of the body immune system (when your immune system mistakenly attacks its own healthy cells or tissues). About 30 percent of all cases are thought as a consequence of immune system abnormality. For such cases, this is also called autoimmune hives.
Autoimmune hives is not fully understood yet. No one knows what causes this abnormality. Interestingly, sometimes it may occur in combination with another autoimmune disorder, such as:



