Exercise and Diet to Treat Chronic Paresthesia in Legs!
Does appropriate diet and exercise can help relieve chronic paresthesia in legs? The answer varies from patient to patient, and typically depending on the underlying cause of the symptoms!
Sometimes medications are necessary. For instance, if the reason is diabetes and patients also have poorly controlled blood sugar, doctors may need to prescribe some insulin replacement to restore or maintain the blood sugar (glucose) as close to the level of normal as possible.
Again, the health condition for the reason of your persistent paresthesia plays a role.
If the cause is multiple sclerosis, for example, your professional trainer needs to make some adjustments to meet your body needs. Multiple sclerosis could be a debilitating condition, affecting your ability to move certain parts of your body.
If the cause is diabetes, do exercise but in moderation. Since people with diabetes are at high risk of experiencing hyperglycemia (a condition of blood sugar level that increases too high) or hypoglycemia (blood sugar level decreases too low), it’s crucial to keep monitoring your blood sugar regularly. Click this section for in-depth information to exercise with diabetes!
And if the reason is poor diet such as lack of dietary vitamin B-12, lifestyle measures including diet and exercise would help a lot.
Ask a professional trainer or your GP for more advice before starting exercise for better result and to keep safe!
What actually are they? They are a group of muscles of the hip joints. They are critically important to help the movement of your hip and knee, such as for crossing your legs, straightening your knee, walking, and running.
If you are physically inactive, this may contribute to cause tingling & numbness in the hips or other parts of your legs. And training your hip flexors properly may help relieve paresthesia in the legs.
Stretching focused to train the hips will help strengthen the muscles of the hips (hip flexors), and this may help improve paresthesia.
The hip flexors are located on the below hipbones and upper thighs. Here are some exercises to train the muscles of your hips:
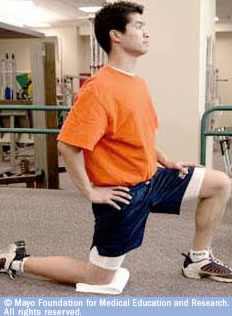
- Gradually kneel your right knee on a pillow or a folded towel.
- Then position the left foot in the front of your body! Bend your left foot. To keep you stable, place your left hand on the left leg!
- Place the right hand on the right hip, don’t bend it at your waist! Tight your abdominal muscles and straight your back!
- Then gradually lean forward, shifting more weight of your body onto the front leg. In this session, you should feel a stretch in the right thigh.
- Hold for about half a minute (30 seconds)!
- Repeat these steps for your left foot.
Repeat this for several times! Check the image below (credit to Mayo Clinic)!
Hip flexion resistance, floor /standing leg raises, or even sit-ups also can help improve the hip flexors. But do these carefully!
We all agree that walking is the easiest exercise – it is simple and practical, you can do it anytime and anywhere. Does it help improve the symptoms of paresthesia? Yes it does, some studies have confirmed the benefits but again, this is also dependent on the underlying cause of the problem.
If the cause is neurological disorder such as multiple sclerosis and stroke, patient may be less likely to get advantage most from walking. Also in several cases, chronic paresthesia in the legs can cause difficulty walking.
If there are some damages of nerves in your legs, you are greater chance of getting loss of balance or even weakness.
If your doctor allows you take moderate walking therapy, choose the level ground to ease your steps when walking. After walking, always check your legs – make sure that there are no sores, redness, or other unusual symptoms in your legs!
When it comes to diet, one of pretty common causes of persistent paresthesia is vitamin B-12 deficiency.
Getting plenty of vitamin B-12 can significantly help improve the problem, particularly true if the major cause of the problem is vitamin B-12 deficiency.
If necessary, doctor may also prescribe some vitamin B-12 supplements (sublingual or oral type) to help restore the deficiency back to normal. What’s more?