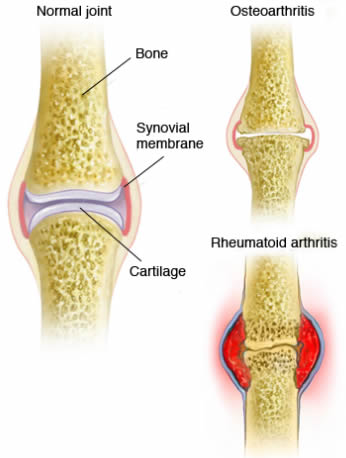
How Does Osteoarthritis Differ From Rheumatoid Arthritis?
There are several forms of arthritis (a common joint disease), some of them are osteoarthritis (OA) and rheumatoid arthritis (RA) – even OA is the most common form. It’s not always easy to distinguish between OA and RA since the affected joint can have the similar symptoms. However, there are some differences.
OA is currently thought as a consequence of wear and tear on the joint as the age. It has nothing to do with the abnormality of body immune system. Sadly, the exact cause is not fully understood yet.
Now experts believe that it is not purely mechanical problem from consequence of years of use. Other factors such as genetics, obesity, trauma, or other factors may have a role.
How about with RA? Like OA, the way of how RA occurs is also unclear yet. Currently, it is thought as a consequence of wrong respond of immune system. In RA, the immune system mistakenly attack healthy tissues, specifically the lining of membranes around the joint – causing the damaged cartilage and bones in the affected joint.
 It’s not clear why the immune system attack its own healthy cells /tissues – though some theories have been proposed. But in general, it thought as a result of a combination of environmental and genetic factors.
It’s not clear why the immune system attack its own healthy cells /tissues – though some theories have been proposed. But in general, it thought as a result of a combination of environmental and genetic factors.
Some studies have shown that some genes may be associated with the development of RA. These include HLA, C5, TRAF1, PTPN22, and STAT4.
Not all people who have these genes develop RA. This suggests that genetic may not play alone. Some studies are continuously going to observe other factors. These may include female hormones (in fact, RA is more common in women), certain viral /bacterial infection, and the respond of the body to stressful events.
While the exact cause behind the problem for both types is not finally confirmed yet, experts have confirmed some factors and conditions that increase the risk of developing OA and RA.
Age and gender are risk factors of both. OA and RA affect more women and tend to occur at the age older than 40 – though RA can occur at any age.
RA is more likely to run in families than OA. If you have a family history of RA, this increases your risk of developing the same problem later in your life. However, certain kinds of OA may also run in families – particularly for OA of hand and finger.
Obesity and physical trauma (such as joint injuries in sport activity) increase the risk of OA, but not for RA. However, these can worsen both OA and RA.
Both OA and RA are difficult to be diagnosed at early stage. Since early diagnosis is essential for the prognosis, some studies are continuously observing the effective method to diagnose them as early as possible.
Physical exam, imaging tests (such X-ray, MRI, or CT scan) and blood test are common procedures used to help doctor diagnose the problem.
If compared to RA, people with OA are less likely to have rheumatoid factor in blood test. On the other hand, many people with RA have this antibody-protein (rheumatoid factor is a protein produced by the immune system that attacks its own healthy cells /tissues) – though not all people with RA have it in blood test.
See also more tests to diagnose osteoarthritis in this section!
Although OA and RA can share some similar symptoms or other characteristics, but they are different types of arthritis!
Each type is treated with different ways – though some medications and therapies may work for both types. So, it is so important for doctor to make a clearly diagnosis of the kind of arthritis that you have!
Since RA is related to the overactive immune system, it is often treated with medications that can help control or suppress the immune system. On the other hand, immunosuppressants are commonly not used to treat OA.
And if other treatments don’t work, both types can be treated with surgery. The severity of the problem can significantly affect the kind of surgery you need to take.
Generally, the cause behind the problem of each type is the main difference.
As written before, OA occurs due to ‘wear and tear’ the cartilage in the affected joint. And for RA, it occurs when the immune system mistakenly attack the synovial membrane in the joint, causing damage to the cartilage and bones within the joint. See the picture below (image credit to Mayo Clinic)!
What else? To clearly understand how osteoarthritis differs from rheumatoid arthritis, the following is a helpful table (see on the next page):