Severe Rheumatoid Arthritis in Hands
Severe RA (rheumatoid arthritis) in hands is commonly found in the joints of fingers and wrists. For other common joints where it occurs, see this post! The next question, how soon the disease will get worse! And what are the treatment options?
The symptoms that are present can be one of major factors to determine the severity of the disease. Doctors usually also need to evaluate the severity of joint damage and physical function!
 In severe cases, RA in fingers and wrists usually come with a high level of pain, swelling, and stiffness. These symptoms can be severe enough to affect the daily activities. Other symptoms may include:
In severe cases, RA in fingers and wrists usually come with a high level of pain, swelling, and stiffness. These symptoms can be severe enough to affect the daily activities. Other symptoms may include:
- Joints of hands and fingers are tender and warm to touch.
- RA is more likely to affect hand joint symmetrically (for instance, on both fingers and hands).
- Flu-like feelings and symptoms may occur, too.
- Stiffness and pain usually last at least about an hour or more.
- Carpal tunnel symptoms. In fact, severe RA (particularly in wrists) often causes complications such as carpal tunnel syndrome.
The deformities in the involved joint (particularly hand deformity) are pretty common in severe RA. If the inflammatory process of the disease is out of control – it could also affect other organs, causing other problems such as weight loss, anemia, fatigue, sweating, and some serious complications (such as heart disease, lung problems, eye dysfunctions, etc.)
So, RA is not a usual joint condition. It is a systemic arthritis. In other words, it can affect your overall health.
Many times, patients ask about what they can expect for the prognosis and how severe the disease will get worse. Most of them are anxious to get to know about the future associated with their RA in the hands and any factors that can affect the prognosis and outlook of the disease.
But there is no single answer for these questions. The prognosis can vary from patient to patient, and each case can be unique. However there are some variables to predict how severe RA will become, these include:
- Like most things in many health conditions, RA is relatively easier to treat when it is diagnosed at early stage and appropriately treated in the first 2 years after the diagnosis. This 2-years mark is still debatable, but some experts believe that this period is very crucial to control and treat the disease.
- How advanced the disease when was first diagnosed can have an effect, too. For instance, significant joint damage may already be found on X-rays when the disease is first diagnosed at advanced stage, and this can affect the kind of the treatment you need to take.
- The currently ‘inflammatory progression’ of the disease itself (how active your RA is currently – whether it is well controlled, in a remission, or in a flare). This may be the most important factor for the prognosis.
- The presence of anti-CCP (anti-cyclic citrullinated peptide antibody) and RF (rheumatic factor) in blood tests. Not all people with RA have these indicators. But for those with anti-CCP and RA, they are more likely to develop severe form of the disease.
- RA is commonly found in those with the ages of 40-60 years old. In a few cases, it is found at young ages. And if you get the diagnosis of your RA at very young age and have had active the disease for many years, you are more likely to have destructive form of RA.
- The presence of rheumatoid nodule. It can be an indicator that you have had RA for years and not well-controlled. See more this nodule in here!
- The presence of elevated inflammatory indicators such as elevated ESR (erythrocyte sedimentation rate) and CRP (C-reactive protein).
The following are other facts you need to know:
- Many sufferers have progressive and chronic RA that make them need to take long-term medical treatment.
- About 10-20 percent of patients with RA experience sudden onset of the disease. Interestingly, the symptom onset is then often followed with many years without any symptom, a period called ‘prolonged remission’.
- And some sufferers experience symptoms that come and go! They can have intermittent RA symptoms, periods of when there are no /few symptoms that strike between flares and last for several weeks or even months.
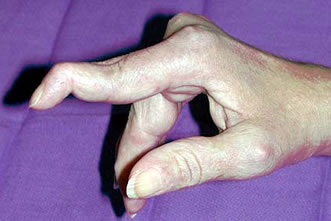
And for RA in hands (especially in fingers), there is a chance for the disease to lead to a swan-neck deformity. It is a condition typically characterized by the middle joint straightens, but the base of the affected finger and the outermost joint bend.
*Image credit to Ortho Bullets
If you have swan-neck deformity, it can be very difficult or even impossible to bend the involved finger in normal movement. Eventually, this may affect your daily routines because you will have trouble to pinch or grip with the affected finger.
A professional rheumatologist can diagnose this complication by observing the affected hand and fingers. For the treatments, these may include: