Differences of Peptic, Gastric, and Duodenal Ulcer!
Peptic ulcers are a medical term used to call a defect that occurs in the lining inside esophagus, stomach, and the upper part of small intestine. A peptic ulcer that occurs locally inside the stomach is called gastric /stomach ulcer. And one that locally affects the first part of the small intestine is called duodenum ulcer. Are there any differences from them?
There is still no clearly cause of this digestive problem. But experts believe that the imbalance’s effect of digestive fluids may have an effect in triggering the problem.
The prognosis of ulcer is pretty good if it is completely cured. If left untreated or incompletely treated, there is a chance for it to return.
Foods that you eat will pass your esophagus and then go into your stomach. The stomach itself can make some acids. These acids are not essential but pretty helpful in digesting the foods you eat. Then foods will be directed to the first part of small intestine (called as duodenum).
After being processed and mixed in the stomach, foods will be mixed with some enzymes in the small intestines. The essential enzymes from pancreas or other parts of the body (such as from cells of the intestine’s lining) will be released to completely digest foods that you eat.
In essence, these enzymes will help digest and break down the food. Then eventually the essential nutrients from the digested foods are absorbed by cells of the body.
There are 3 major possible causes for this kind of digestive problem:
- Helicobacter pylori infection. In fact, many patients who develop peptic ulcers also have H-pylori infection.
- The excessive consumption of painkillers.
- A health problem (such as gastrinomas, tumor) that triggers the over production of acid fluid.
The following are some conditions that increase the risk of developing peptic ulcers:
- Having H. pylori bacterial infection.
- Age, in other words your risk increases as you age!
- Frequently drinking alcohol too much.
- Having other serious diseases that affect your digestive system, such as diseases of lung, kidney, and liver.
- Taking pain killers such as naproxen, aspirin, and ibuprofen (especially too much consumption of these medications).
Moreover, some experts believe that having a family history of peptic ulcer is also another risk factor – though there are also a few studies found that it may not run in the families.
There is no significant difference for the risk factors, the theories of possible causes, and the symptoms of between duodenal and stomach ulcers. Even in making diagnosis of both conditions, doctors often use the same procedures [reference].
As mentioned before, the major different thing for both digestive problems is the location of where the ulcer occurs.
Below is the image (credit to Mayo Clinic) of the location for each type:
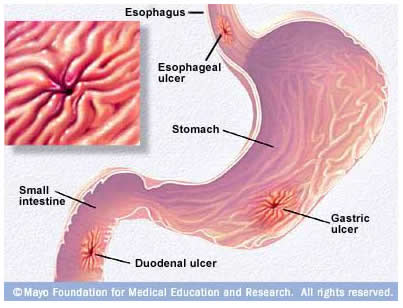
Stomach ulcer is less common than duodenal ulcer (the most common type of peptic ulcer)! The common signs and symptoms of both conditions may include:
- Abdominal pain, which is usually the most common symptom.
- Bloating, heartburn, nausea & vomiting.
- In severe case, there is a chance for patient to have bloody stools in a bowel movement or bloody vomiting.
What’s more?




WHICH FOODS ARE EAT BY A PEPTIC DUODENAL ULCER PATIENT
#SKDASH
The kinds of foods for duodenal ulcer treatment may vary from patient to patient. This link may help!
Thx